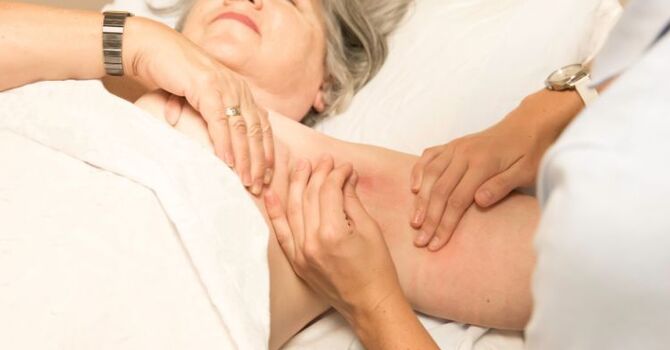
Living with lymphedema means dealing with persistent swelling, heaviness in your limbs, and the way it chips away at everyday movement. What many people don't realize is that physical therapy for lymphedema is one of the most clinically supported ways to reduce that swelling and restore function. At Salt + Light Wellness in Reno, NV, this is work we do every day, and the results are meaningful when treatment is done right.
Here's a clear, honest look at how physical therapy addresses lymphedema, what the science shows, and what you can realistically expect.
What the Research Actually Shows
The gold-standard treatment for lymphedema is called Complete Decongestive Therapy, or CDT. It brings together four components: manual lymphatic drainage (MLD), compression therapy, therapeutic exercise, and skin care. Research published in journals including Lymphology and the Journal of Clinical Oncology consistently shows that CDT can reduce limb volume by 30 to 60 percent during the intensive treatment phase — particularly in patients with breast cancer-related lymphedema.
Clinical guidelines from the International Society of Lymphology identify CDT as the leading conservative treatment for lymphedema. This isn't an experimental approach. It's a well-established, evidence-based protocol that specialized physical therapists are trained to deliver.
How Manual Lymphatic Drainage Moves Fluid Out of Affected Tissue
Manual lymphatic drainage is the cornerstone of CDT, and understanding how it works helps explain why it's so effective.
The lymphatic system relies on a network of vessels just beneath the skin that transport protein-rich fluid back into circulation. When these vessels are damaged or blocked, fluid accumulates in the surrounding tissue and causes swelling. MLD addresses this through several specific physiological mechanisms.
Stimulating lymphangiomotoricity is the first. Lymphatic vessels have the ability to contract rhythmically on their own, pumping fluid forward through the network. MLD uses precise, gentle, rhythmic skin movements to stimulate these contractions and increase the rate at which fluid moves through the system.
MLD also works by opening collateral lymphatic pathways — essentially rerouting fluid around damaged or blocked areas and directing it toward intact lymph node basins such as the axillary, inguinal, or supraclavicular regions where it can be properly processed.
At the tissue level, MLD reduces interstitial fluid pressure. When pressure in the tissue drops, the conditions improve for excess fluid and proteins to re-enter the lymphatic capillaries. This is why the technique uses very light pressure rather than deep compression. Lymphatic capillaries sit just beneath the skin and respond to gentle stretching of the skin surface, not deep tissue pressure. Applying too much force actually collapses the vessels rather than opening them.
You can read more about the physiological basis of lymphatic drainage through the Lymphatic Education and Research Network.
The Mobility Improvements You Can Expect
When lymphedema swelling decreases, the functional gains that follow are often significant. Patients commonly experience increased range of motion in the affected joint — whether that's the shoulder, elbow, hip, knee, or ankle. Walking tolerance and endurance improve. Overhead reaching, lifting, and daily tasks that previously felt impossible become manageable again.
Beyond joint mobility, patients typically report a reduction in the characteristic heaviness and tightness in the affected limb. Balance and coordination often improve as well, particularly when lymphedema has been affecting gait. The overall ability to participate in exercise and daily activities increases — which matters not just for physical function but for mental wellbeing.
There's also the connection between swelling and nerve symptoms. When lymphedema goes unaddressed, the accumulated fluid creates mechanical pressure on surrounding nerves and structures. At Salt + Light Wellness, we work regularly with patients experiencing both lymphedema and neuropathy together, and reducing the fluid load in the tissue often has a direct positive effect on pain and sensory symptoms.
Why Leaving Lymphedema Untreated Makes It Harder to Manage
Lymphedema is not a stable condition without intervention. It tends to progress, and the longer treatment is delayed, the more complex management becomes.
Without treatment, limb volume continues to increase. Over time, the accumulated protein-rich fluid triggers a process called fibrosis, the tissues begin to harden and thicken, becoming progressively more resistant to treatment. Skin changes like hyperkeratosis and papillomas can develop. The risk of recurrent infections, particularly cellulitis, increases significantly because the stagnant fluid creates an environment where bacteria can take hold. Chronic pain and heaviness become more entrenched. In severe long-standing cases, a rare but serious complication called lymphangiosarcoma, a cancer of the lymphatic vessels — has been documented.
Early treatment matters because lymphedema is considerably easier to manage in its earlier stages, before significant tissue changes have occurred. If you've noticed swelling that persists or worsens, getting a proper evaluation sooner rather than later gives you the best possible outcome.
What to Look for in a Lymphedema Therapist
Not every physical therapist is equipped to treat lymphedema. The lymphatic system requires specialized knowledge and hands-on technique that goes well beyond standard PT training.
Look for therapists who hold a Certified Lymphedema Therapist (CLT) credential, or ideally a CLT-LANA designation awarded by the Lymphology Association of North America. These certifications require advanced coursework and clinical training in manual lymphatic drainage technique, compression bandaging and garment fitting, lymphedema-specific exercise prescription, and skin care and infection prevention protocols.
Working with a trained specialist matters both for safety and for outcomes. Poorly applied compression or inappropriate massage technique can worsen symptoms rather than relieve them.
Building a Long-Term Management Plan
Because lymphedema is a chronic condition, the goal of physical therapy isn't just to reduce swelling once, it's to give you the tools to manage it over the long term. A well-designed program includes a home exercise program using gentle rhythmic movement to activate the muscles around the lymphatic vessels and support natural fluid pumping, self-drainage techniques you can apply daily, skin care protocols to reduce infection risk, and clear guidance on when to seek additional support.
Compression garments fitted as part of your program help maintain the gains made during treatment by preventing fluid from re-accumulating between sessions. Your therapist will make sure you understand how to use them correctly and how to adjust your approach as your condition changes.
Ready to Get Started?
If swelling has been limiting your movement or your quality of life, physical therapy for lymphedema offers a clinically grounded path forward. The team at Salt + Light Wellness in Reno brings specialized lymphedema training to every session, with an approach that addresses the whole person.
Reach out to us to schedule a consultation and find out what a personalized lymphedema program could look like for you.